DESPERATE to end the extreme bloating and crippling pain she had suffered for years, Sarah Garlick accepted extreme measures.
Aged just 40, she underwent a hysterectomy which plunged her into surgical menopause.
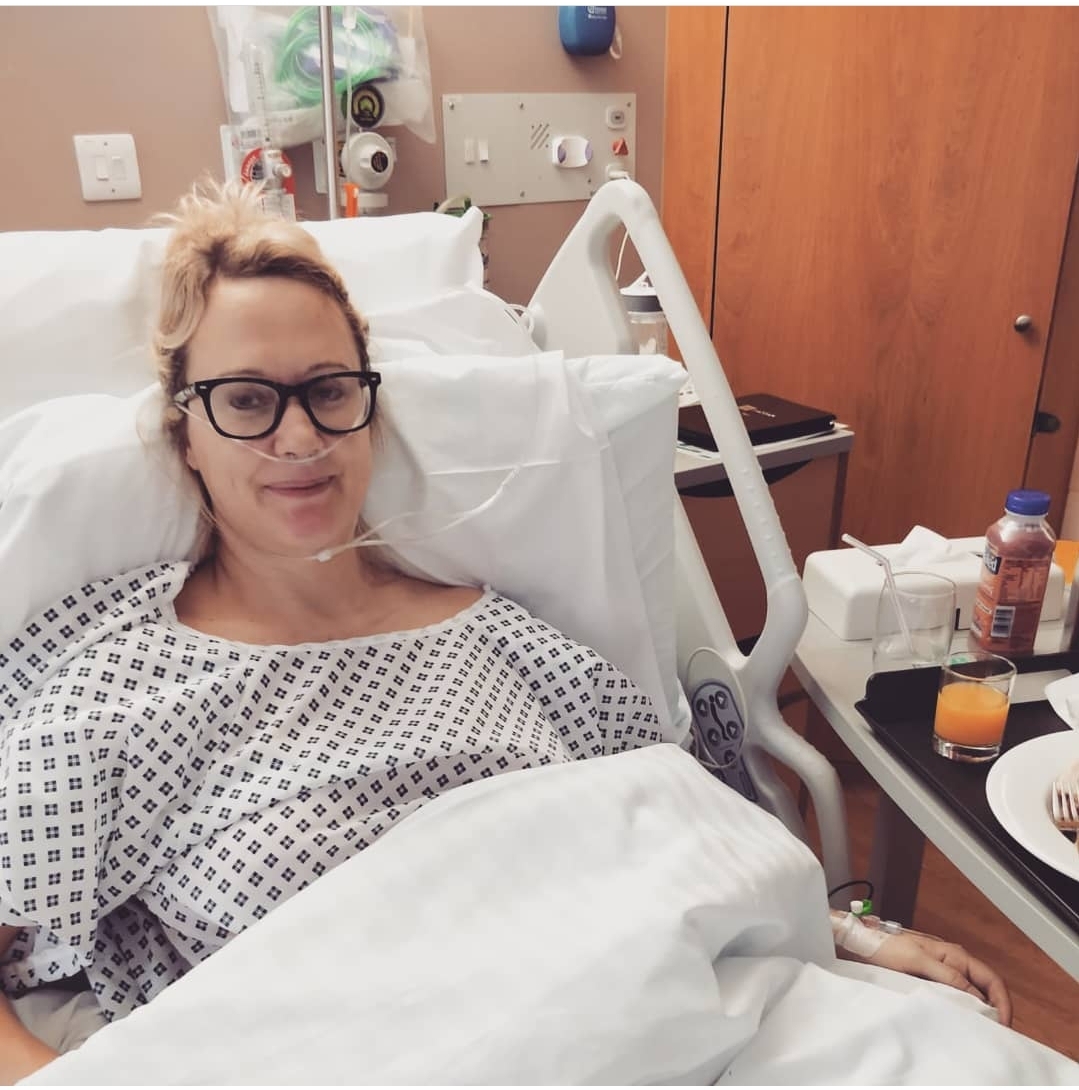
Sarah Garlick underwent a hysterectomy to cure severe bloating, only to later find out her colon was the issue, not her womb
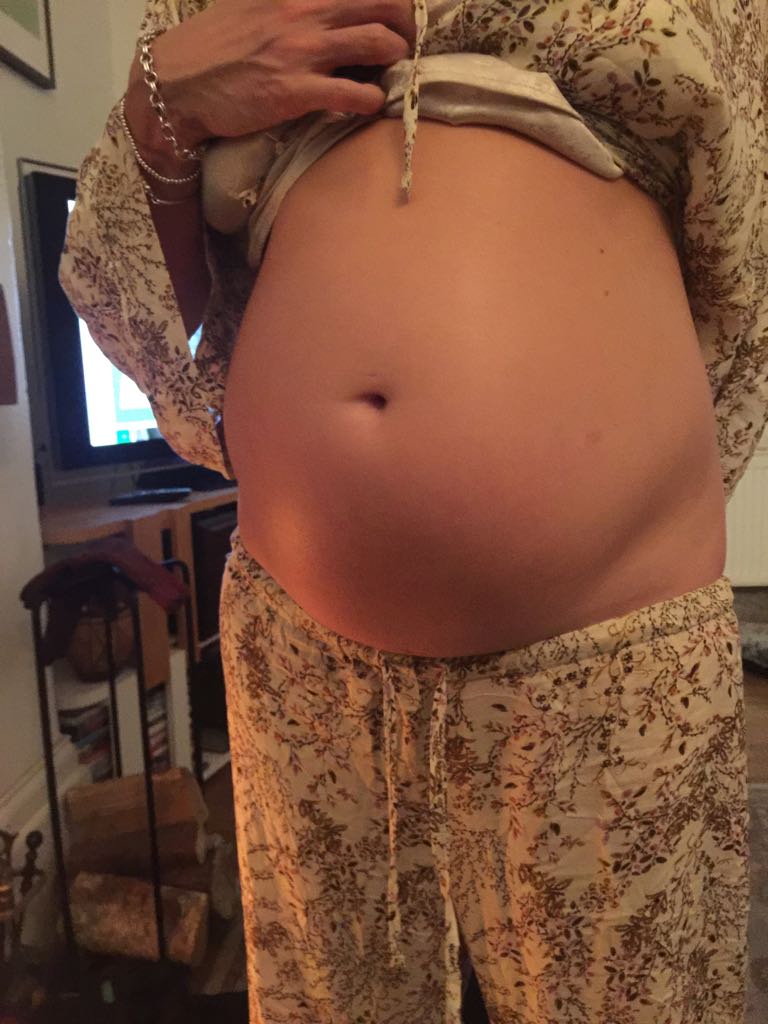
Sarah’s condition leaves her with crippling pain and extreme bloating
The now 46-year-old was so sick of being “fobbed off by doctors” who had misdiagnosed her with irritable bowel syndrome, and felt she had no choice but to have the op.
She was forced to wear maternity clothes, and could go from being a size 10 to looking nine months pregnant within the space of 30 minutes when she had an “attack”.
However, when Sarah, from Portishead, Bristol, recovered from the hysterectomy and her symptoms returned, she realised the drastic measure that changed her life hadn’t solved her bloating problem at all.
It took another five years for Sarah to get a final diagnosis; that she was suffering with a ‘torturous colon’, which is when the colon becomes too long and thin, making digestion difficult.
“I looked as though I was about to give birth, my stomach would swell, and I would be doubled over in pain.
“It would last for hours and I had no idea what was causing it. The GPs didn’t know either,” Sarah told Sun Health.
“So when after hundreds of GP appointments and tests, I was advised my best option was to have a hysterectomy, I thought I had no choice. I wanted to get my life back.
“When the bloating returned with a vengeance after my operation and battling with surgical menopause, I felt like giving up. I couldn’t believe it.
“After more tests, I was told I had a ‘tortuous colon’, and that meant I needn’t have had the hysterectomy.
“I’ve overhauled my diet, cutting out sugar, which can trigger attacks, and am taking supplements and I’m in the best shape I’ve been in for years.”
Sarah’s problems started in 1987 when she started her periods, which would leave her ashen, bedridden, suffering with migraines and mentally devastated every month.
At 15, after numerous visits to her GP, Sarah was put on the contraceptive pill, which helped control her periods, but still left her in pain.
At 26, after giving birth to her son George, now 20, in 2002, Sarah had the mirena coil fitted as doctors advised it was an ‘upgraded’ form of contraception.
Sarah was a single parent for eight years and later returned to university to train to be a counsellor and now helps students with mental health issues at The University of the West of England.
She then met her now-husband, Paul, and they got married in 2012 when she was 36.
She had the coil removed as the couple were considering having more children.
She said: “Everything was fine, until my old teenage symptoms came flooding back.
“After a year of marriage, my periods were still horrendous, so the GP referred me to gynaecology and an endometrial ablation was recommended.
IN AGONY
“The ablation meant I would be unable to fall pregnant. I was in so much pain, so I had the operation at 37 and we knew we would never have a child together.”
The ablation was a shock to Sarah’s system and there was a devastating increase in pain.
This was when Sarah first started experiencing severe bloating. Nothing seemed to trigger it, she kept food diaries and activity diaries – but there was no pattern.
In 2016 doctors recommended Sarah undergo a hysterectomy, believing it to be the cause of her symptoms.
Sarah said: “The time in between the bloating became worse. It was only a month after the ablation that the bloating returned.
“I also still had periods which were insanely painful.
“Doctors suggested a hysterectomy and I learned this was ‘just’ the removal of my troublesome womb.
“The consultant confidently informed me that Adenomyosis cells had been found in my old tired womb and that this had been the cause of my swelling and bloating.
“I felt relief as at last I had a reason for the bloating.”
However, two months after the operation, Sarah was left horrified when the bloating returned.
Back to her GP, Sarah was referred to gastroenterology.
She added: “This time, my ‘ghost womb’ ramped up the bloating. I was spending more days in bed, surgically attached to my heat pad. I started to run out of things to watch on Netflix.
“I was in maternity clothes. I could go from a size 10 to a nine month pregnant woman with twins in the space of 30 minutes.
“I started to miss more of my life. I was put through myriad tests. There was some talk, after a session of ‘biofeedback’ that my pelvic floor was too tight.
“As well as a tear-jerking, endoscopy and colonoscopy, I also had a functional gut test.”
Sarah was given a “vague diagnosis” of irritable bowel syndrome and prescribed medication in 2016.
She was also referred to a gynaecologist who administered Zoladex implants and chemical menopause ensued.
The implant slowly releases hormones into the body after it is placed by injection under the surface of the skin of the stomach.
It works to lower levels of sex hormones such as testosterone and oestrogen.
The implant itself will be completely absorbed into the body over weeks or months.
It is generally used as a therapy option for patients with breast cancer, prostate cancer, or endometriosis.
Professionals explained that the idea was to “turn off” her ovaries to see if that helped her bloating – but without HRT.
Sarah said: “The Zoladex implants seemed to have fixed things but my mental health was collapsing – I was in possession of a relentless, racing, distressed and confused mind.
“No matter how much I tried to explain that chemical menopause is different to the natural run up, people didn’t seem to understand.
“That Christmas, the Zoladex implant was due to wear off and I thought the day could double up as a joyous end to chemical menopause.
“But right on cue, the bloating returned. By Boxing Day, I was in unbearable pain, desperately seeking comfort in a hot bath like a birthing hippo.”
Incredibly frustrated, Sarah jetted off on holiday and it was while lying by the pool that she took a photo of her tummy in a bikini.
She created her Instagram account @Terrible_Tum, in a last desperate plea to fix things.
She said: “I have found the state of women’s healthcare is nothing short of a global scandal.
“Receiving messages of support from strangers who know exactly what you are going through is balm for the soul. It’s the best kind of women supporting women.”
In spring 2019, Sarah visited a specialist consultant in Birmingham and was told the latest plan was to remove her ovaries, her cervix and any endometriosis and remaining adenomyosis cells.
So at 43 in 2019, she underwent bilateral salpingo oophorectomy surgery.
She recalled: “Surgical menopause was not mentioned much. At 43, with no more children to bear, my ovaries were whipped out and I have a ‘cuff’ instead of a cervix.
“I remember the consultant visiting to say all went well. But he let me know that if the terrible bloating came back, there would be nothing further that could be done.”
For a year after the operation, Sarah battled to get the right dose of HRT that made her feel most like herself.
‘FAMILIAR TWINGE’
But, a year later in July 2020, her bloating and pain returned.
Sarah said: “I was working a duty shift, sitting at my desk looking out at the sun, when I felt the familiar twinge and stabbing pain return.
“I felt numb. I even had to locate the maternity clothes I thought I had put away forever.
“The GPs didn’t know what was wrong so morphine was prescribed.
“The pain was excruciating and unbearable. I was referred to Gynae and warned the waiting list was awful.
“Meanwhile I was always suffering; I spent days and weeks in bed. The bloating was constant – it never left.”
Sarah finally received her appointment in March 2021 but the gynaecologist said there was ‘nothing that could be done’ as she had no gynaecological organs left.
Sarah underwent more tests with a colorectal surgeon and it was revealed she had a ‘tortuous colon’ – when the colon becomes too long and thin, making digestion difficult.
They suggested a stoma bag to see if it helped her intestines and the bloat. But Sarah is not sure she can bring herself to have another operation.
Meanwhile, Sarah’s husband met a man in the pub who was convinced he’d be able to help reduce Sarah’s symptoms.
Clued up on diets and supplements he suggested vitamin C, vitamin D and magnesium, as well as cutting out sugar, could help Sarah.
With few options remaining, Sarah decided to give it a go.
And miraculously, his advice worked. Sarah still has the capacity to bloat but she can finally control it more. Her surgeon is amazed.
Sarah said: “I cannot lie, I wish I had kept one ovary. I wish I had known. And now I have started a menopause support group called menochat – to help others.
“It’s frustrating to know I needn’t have gone through that hell and all those operations.
“I’m devastated but I’m determined to help others.
“Changing my diet completely – changing the oils I use to cook with, cutting out sugar and making these changes has helped more than anything has ever helped. It is remarkable.
“I still have the capacity to bloat – I can still balloon before people’s eyes. But I can control it more.
“I am still pursuing other avenues and the stoma option hasn’t gone – but for now, I’m focusing on helping others and raising awareness.”
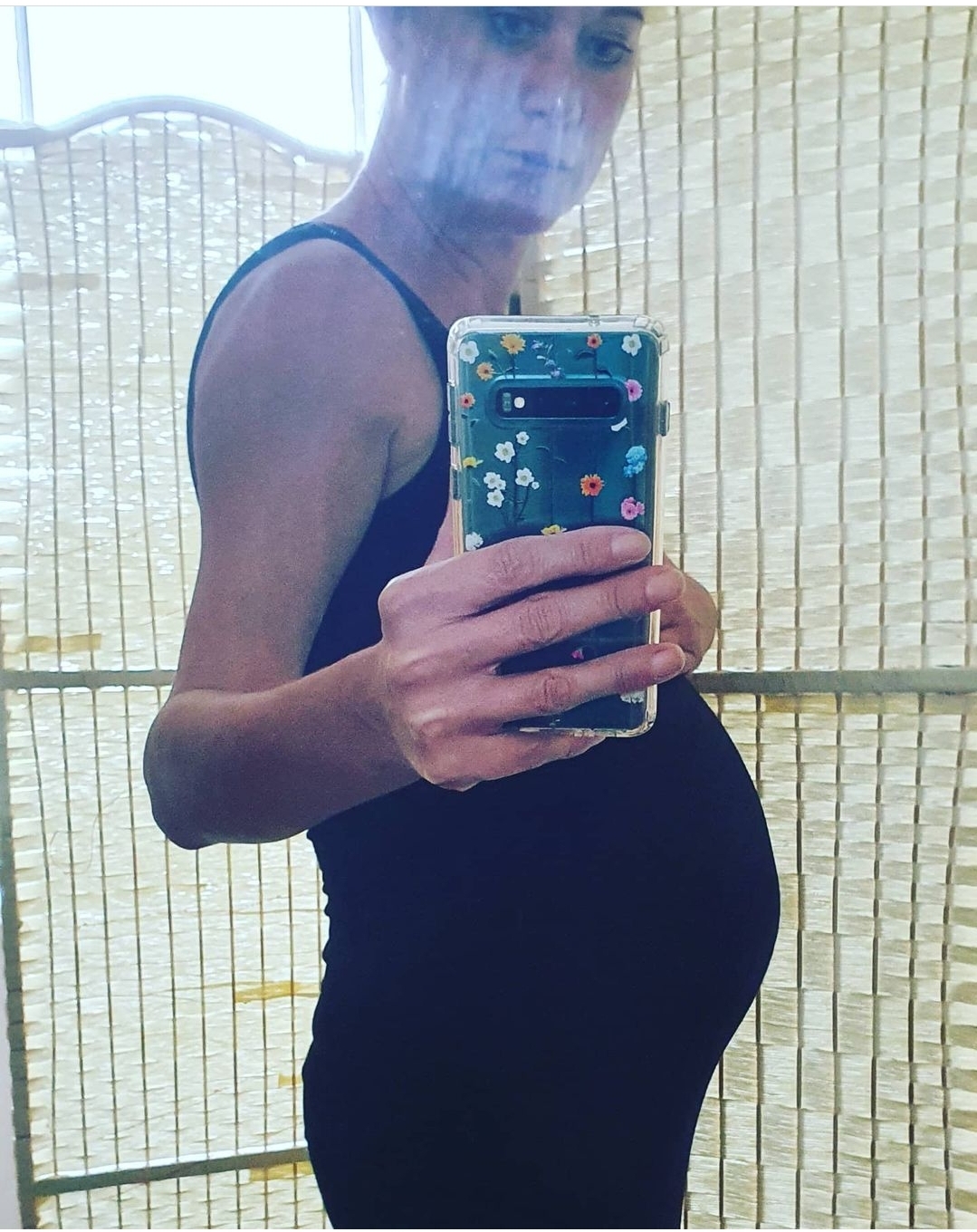
Within half an hour Sarah can bloat so much she looks pregnant

Sarah is now using diet and lifestyle changes to manage her torturous colon